Sexuality and prevention
There are many options at your disposal to avoid sexually transmitted and blood-borne infections (STBBIs).
The most important is regular STBBI testing. Condoms are still a very reliables way to reduce the risk of contracting STBBIs such as HIV. And, if you have been diagnosed with an infection, your strategies may include telling your partners in order to break the chain of transmission, along with a whole range of other things to make your sexual encounters as safe as possible.
- Getting tested
Testing is a very effective way to know if you have a sexually transmitted or blood-borne infection (STBBI) or the human immunodeficiency virus (HIV). Once you have been diagnosed, you can then be treated and cured, or begin the necessary medical care if you find out you are HIV-positive.
Why should I get tested?
You have never been tested, are starting a new relationship, had sex without a condom, or are pregnant or trying to get pregnant? Getting tested for HIV and other sexually transmitted and blood-borne infections (STBBIs) is the only way to detect an infection and get access to medical care and support if you need it
It is confidential and free! Because these infections don’t always have symptoms/can often go undetected getting tested will give you peace of mind and keep you and your partners healthy.
How often should I get tested?
How often you get tested depends on several factors. The most important thing to remember is that getting tested regularly is the best way to quickly detect an infection.
You should think about getting tested if:
- You have a new sexual partner
- You have multiple sexual partners
- You have had sex without a condom
- You use drugs
- You want to get pregnant
Be proactive. Talk to your doctor. You do not need to wait until he or she brings it up to ask for information about getting tested for HIV and other sexually transmitted and blood-borne infections (STBBIs). It is important to be able to speak openly and unreservedly with your healthcare professional. The more they know, the better they will be able to determine what tests you need, and how often you should get tested.
Where and how to get tested?
There are many places where you can get tested for HIV and other sexually transmitted and blood-borne infections (STBBIs). Every region of Quebec has at least one CLSC offering HIV and STBBI testing. Your local community HIV organization may even offer this service. For more information on the services offered in your area, refer to the Where can I get tested?
Testing is confidential and free for anyone with a RAMQ Health Insurance Card. It only takes a few minutes. Testing involves a blood test and may involve other exams such as giving a urine sample.
You can get tested as of age 14 without parental consent.
How is the test done?
You will generally have to meet with a doctor or nurse. Before taking samples, they will usually ask you a few questions to determine which tests to perform. Some of us may feel shy about revealing the number of sexual partners we have had or the type of sexual activities we engage into. Know that anything said during the appointment with the healthcare professional is confidential. The more precise the information you share with your doctor or nurse, the better they will be able to assess which tests are needed.
Next, the doctor or nurse will take samples: this generally involves a blood test, urine test, and swabs from the vagina, throat, and/or anus, for example
The results of the tests are generally communicated by phone, with the exception of HIV which requires you to return to the clinic for a second visit to hear the results.
There is also the possibility of doing a rapid HIV test. This test is not free, and is typically offered only in specialized clinics. You will get results from this test on the same visit. If you are interested in this option, ask about its availability when you arrive at the clinic.
What if I don’t have a Health Insurance Card?
A Health Insurance Card is generally necessary to get tested for HIV and other sexually transmitted and blood-borne infections (STBBIs).
If you do not have a Health Insurance Card, visit your nearest CLSC. Many CLSCs will see you even without a card. In addition, they can provide you with information on how to get one.
Anonymous testing is a second option, since this does not require you to show your Health Insurance Card or any other piece of identification. This service is offered in at least one CLSC in each administrative region of Quebec. This service is not offered automatically, you will need to ask for it when you make your appointment.
There is also Médecins du Monde Canada which provides services to certain populations, including refugees and the homeless.
I got tested… Now what?
What if the results are negative?
If your results are negative, it does not mean that you are immune, and will never get an STBBI. Your healthcare professional will discuss with you the strategies to keep up or put in place to reduce the risk of a new infection, or of contracting HIV. In addition, they will let you know when you should get tested again.
What if I test positive for an STBBI
Your healthcare professional will provide you with treatment that should eliminate the infection fairly quickly. Most STBBIs can be treated with medication. For treatment to be effective, you must take every dose, even if you have no symptoms. It is recommended to abstain from sex through the duration of treatment.
Some infections, like herpes and the human papilloma virus (HPV) cannot be cured. However, with herpes for example, there are treatments to relieve symptoms, reduce the duration and frequency of flare-ups, and lower the risk of transmission.
What if I test positive for HIV?
Today, HIV treatments are more effective than ever. The life expectancy of a person living with HIV is nearly as long as the life expectancy of an uninfected person. The more rapidly the infection is detected and controlled after a person is infected, the better their chances of living a long, healthy life. Effective treatment can also greatly reduce the risk of transmitting HIV. Knowing your HIV status is a good way of maintaining your health and protecting your partners.
After diagnosis, you will have regular check-ups in order to control the infection and stay healthy.
HIV treatment is covered by both private and public (RAMQ) health insurance.
Should you disclose your HIV status?
Telling someone that you are living with HIV can be stressful. It is impossible to predict how the other person will react. As a result, the vast majority of women living with HIV are selective about whom? They disclose to, and when. For more information about disclosure or non-disclosure of your HIV status, refer to the site Pouvoir partager / pouvoirs partagés (French).
Choosing to disclose your HIV status involves real risks. In spite of scientific advances in the treatment of HIV, social prejudices have not changed very much. Discrimination, rejection, and even the criminalization of people living with HIV are still real challenges. And the fear that people living with HIV experience as a result of these realities is legitimate.
There is no magical, one-size-fits-all answer when it comes to deciding whether to disclose that you are living with HIV. The rule of thumb is to act with integrity, and make decisions that will allow you to protect yourself, and allow your partners to make informed decisions. One thing is certain, the decision to have sex and the responsibilities that come with it, whether you use protection or not, rests equally on both partners. This moral obligation on the part of both partners is widely recognized throughout the HIV community. However, legally, you should know that you could be prosecuted for failing to disclose your HIV-positive status to your partner.
- Blood HIV self-test (INSTI)
The HIV blood self-test is a test you do yourself, wherever you choose: no need for a prescription or an appointment with a healthcare professional.
WHAT IS THE HIV BLOOD SELF-TEST?
The INSTI® HIV blood self-test analyzes a drop of your blood to detect HIV antibodies and provides a result within one minute.
This test is designed to detect HIV only. It cannot detect other STBBIs such as gonorrhea or syphilis.
You can take the test on your own at home, with a friend, or with the support of a community worker from Quebec’s community HIV network. Simply contact the HIV community organization nearest you to find out what type of support is available.
How does the test work?
The self-test kit includes a detailed, illustrated instruction booklet. You also have access to a video that walks you through the different steps of the self-test.
Instructions:
- Start by washing and drying your hands. Also wash the surface where you will perform the test.
- Prick the tip of your finger with the tool called a “lancet” to draw a drop of blood. Be sure to read the tips in the booklet to make this step easier.
- Add a drop of blood to vial 1 (the red bottle), making sure your finger doesn’t touch the vial.
- Put the cap on and shake the vial. Pour the contents into the provided test container and wait for the liquid to disappear (this takes a few seconds)
- Take vial 2 (the blue bottle) and shake it. Pour the contents into the same container and wait a few seconds for the liquid to disappear
- Take vial 3 (the gray bottle) and shake it. Pour the contents into the same container and wait a few seconds for the liquid to disappear
This process detects what are known as HIV antibodies. These antibodies defend the body against the virus from the onset of infection. It may take 3 to 12 weeks (21 to 84 days) before the body produces enough antibodies for them to be detected by the self-test.
How do you interpret the results?

A single blue dot at the top of the circle: negative test
If you see one blue dot at the top of the circle, the test did not detect HIV antibodies and the result is negative.
Two blue dots: positive test
If you see two blue dots, the test did detect HIV antibodies and the result is positive. In that case, you must see a healthcare professional for a blood test to confirm the result.
No dot or one dot at the bottom of the circle: invalid test
If you do not see any dots or there is only one dot at the bottom of the circle, the test result is invalid, and you will need to repeat the test using a new self-test kit.
Whatever the result, the self-test must never be reused, as it is for single use only.
What should you do if the result is positive?
A positive HIV self-test result must always be confirmed with a standard blood test at a clinic. Check the map of testing locations to find a place near you.
Getting a positive result is not easy, even though people can now live comfortably with HIV. If possible, reach out to someone you trust for support. You can also contact the community HIV organization nearest you for psychosocial support or help navigating the healthcare system.
While waiting for the result to be confirmed, choose with your partner or partners the most effective prevention methods to avoid possible transmission of the virus.
When should you take the test?
The INSTI® self-test should be used between 3 and 12 weeks after a possible exposure to HIV.
Why wait? Because the test can only detect HIV once your body has produced enough antibodies. In some cases, this may happen after 3 weeks, but in others it may take up to 12 weeks.
For example, if you think you were exposed to HIV on June 1, you should wait at least 3 weeks before taking the self-test, so from June 22 onward.
If the result is negative, it is recommended that you repeat the test, using a new kit, 9 weeks later (around August 24) to confirm the result.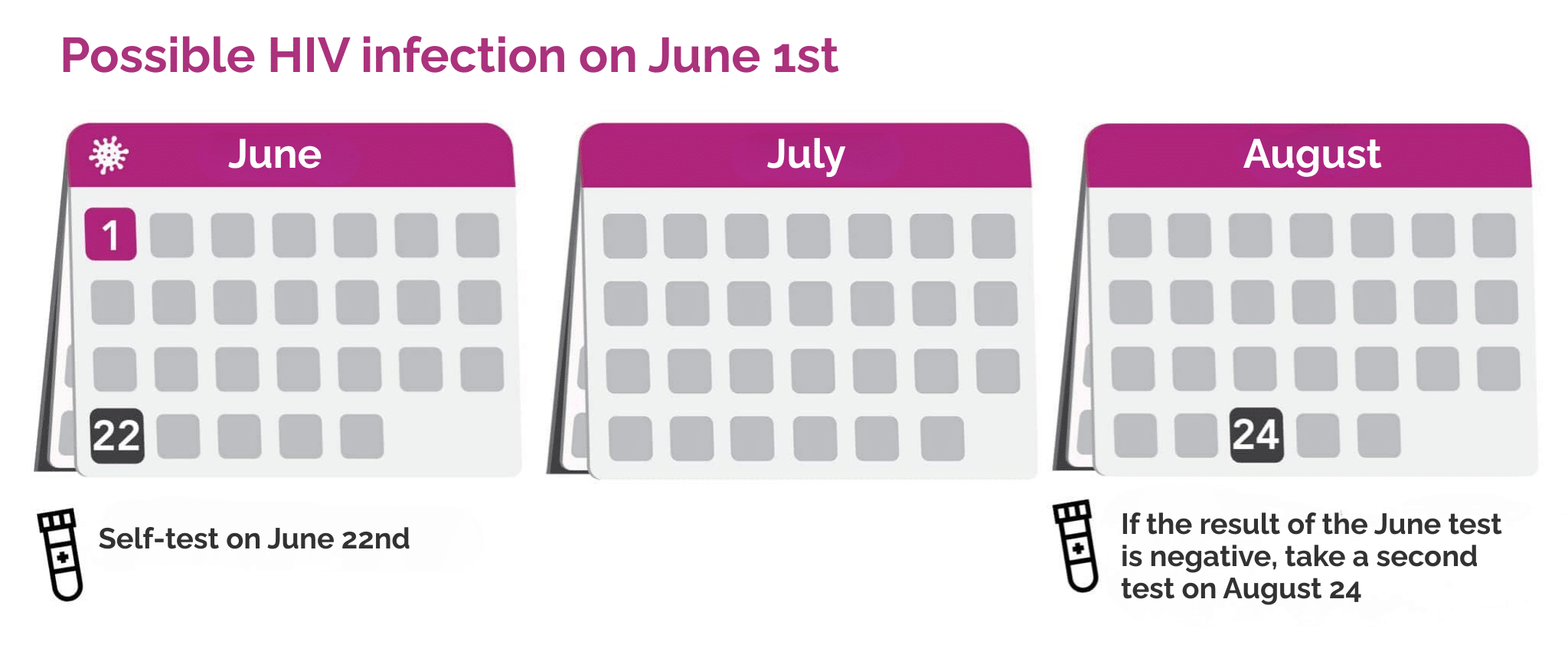
If the self-test result is positive, there is no need to repeat the self-test. Instead, make an appointment with a healthcare professional for a confirmatory blood test.Possible HIV exposures include:
- anal, frontal, or vaginal sex without a condom with a partner living with HIV whose viral load is detectable, or with a partner whose HIV status is unknown;
- sharing equipment used for drug injection.
Should you do it alone or with support?
One of the benefits of the HIV self-test is that you can choose how you want to do it: on your own, at home, with someone you trust, or with the support of a community worker.
A community worker can guide you through the process, help you interpret the result, and support you afterwards if needed.
Support options vary from one organization to another and may be available online, by text, by phone, or in person.
To find support near you, use the postal code search tool to locate the nearest community HIV resource.How can you get an HIV blood self-test kit?
You can purchase the INSTI® HIV self-test kit directly from the BioLytical website, the company that manufactures the test.
The cost is approximately $35 per kit, plus shipping and sales tax, for a total of about $57. Two tests cost approximately $85, including shipping and taxes. The kit can be delivered to the mailing address of your choice.
Until recently, a Canadian program made it possible for community HIV organizations to distribute self-tests free of charge. Unfortunately, that program has been discontinued, and most organizations no longer have enough kits for large-scale distribution. However, you can still contact the organization nearest you to see whether any tests are still available.Blood self-test or oral self-test?
You now have a choice between a blood self-test and an oral self-test. A second HIV self-test was approved by Canadian health authorities in February 2026. Known as OraQuick®, this test uses a sample taken from the gums.
Learn more about OraQuick® below! - Oral HIV self-test (OraQuick)
The OraQuick self-test is a do-it-yourself test used to detect HIV. It analyzes a sample taken from the mouth and provides a result in 20 minutes. It is easy to use, needle-free, and highly accurate (99%).
IMPORTANT: HIV is not transmitted through the fluids found in the mouth.
The self-test detects HIV antibodies, which are what the body produces to defend itself against the virus. It does not detect the virus itself. Since the virus is not present in oral fluids, there is no risk of transmission through those fluids.
It can take up to 3 months (12 weeks) for the body to produce enough antibodies to be detected by the self-test. For that reason, the self-test should be used 12 weeks after a possible exposure to HIV.
Note: This test is designed to detect HIV only. It does not detect other STBBIs such as gonorrhea or syphilis.
How does the test work?The OraQuick self-test is done by swabbing the upper and lower gums with the flat pad of the test device, then waiting 20 minutes for the result. There are three main steps: getting ready, doing the test, and reading the result.
Keep reading for detailed instructions, or watch the short explanatory video produced by COCQ-SIDA.
Getting ready for the test

Here are the steps to get ready:
- 30 minutes before: do not use mouthwash, toothpaste, or teeth-whitening products
- 15 minutes before: do not eat, drink, or chew gum
- Carefully read the instructions included with the test
- Remove any dental device that covers the gums, such as dentures or Invisalign-style appliances
- Make sure you have a way to time the 20-minute waiting period
- Wash your hands
Doing the test
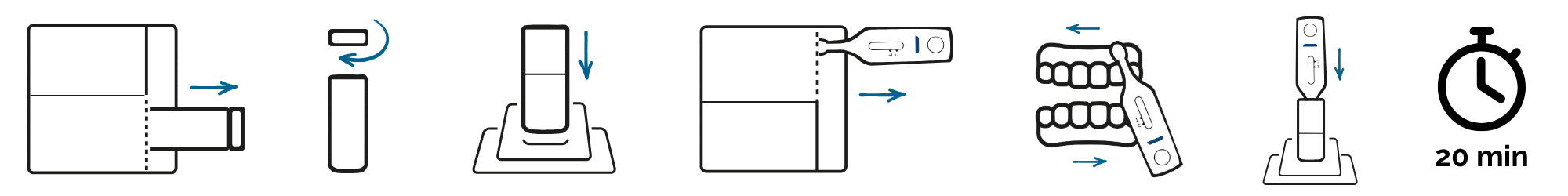
Open the box and place all the items in front of you. The kit contains two pouches attached together.
- Remove the bottle from the bottom pouch first, open it, and place it in the bottle stand
- Remove the test device, following the direction of the arrow
- Be careful not to touch the flat pad with your fingers
- Swab the flat pad along the upper gums, then along the lower gums
- Insert the flat pad into the bottle until it reaches the bottom
- Wait 20 minutes
Reading the results
- After the wait, you have another 20 minutes to read the result
- After that time, the result shown will not be reliable.
Disposing of the test
The test and all of its components can be disposed of in a regular garbage bin.
How do you interpret the result?On the test device, you will see two letters: C for Control, and T, for Test.
As with pregnancy tests, a line must appear next to the C to show that the test worked properly.
Negative result

- One line at the top, next to the C
- No line at the bottom, next to the T
- This means the test did not detect HIV antibodies; the result is negative
Important: if you took the test less than 12 weeks after a possible exposure to HIV, a negative result does not necessarily mean that you do not have HIV. It may simply mean that the test could not yet detect the antibodies because they are still developing. In that case, you should repeat the test once the full 12 weeks have passed to confirm the negative result.
Positive result
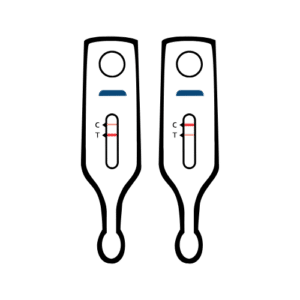
- Two full lines, one next to the C and one next to the T
- Even if one of the lines is faint, it is still valid as long as the line is complete. Partial lines, however, mean the result is invalid (see below)
- This means the test did detect HIV antibodies; the result is positive
You must make an appointment for a standard blood test at a clinic to confirm the result.
Invalid result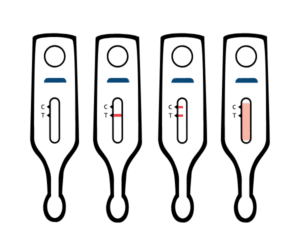
The test is invalid if:
- No line appears
- Only one line appears next to the T, and none appears next to the C
- One or two partial lines appear (one next to the C and/or one next to the T)
- A large red background appears with no lines
An invalid result means the test did not work properly. The result cannot be interpreted, and you will need to repeat the test using a new kit. Do not reuse the same test.
What should you do if the result is positive?
A positive HIV self-test result must always be confirmed with a standard blood test at a clinic. Check the map of testing locations to find a place near you.
Getting a positive result can be difficult, even though people can now live comfortably with HIV. If possible, reach out to someone you trust for support. You can also contact the community HIV organization nearest you for psychosocial support or help navigating the healthcare system.
While waiting for confirmation, choose with your partner or partners the most effective prevention methods to avoid possible transmission of the virus.
Is OraQuick right for you?OraQuick is intended for anyone who is HIV-negative and thinks they may have been exposed to HIV, EXCEPT:
- people taking antiretrovirals such as:
- PrEP: if you are taking PrEP, it is recommended that you go to a testing site and take a standard blood test instead
- PEP: if you are taking PEP, it is recommended that you follow the advice of the healthcare professional who prescribed it and take a standard blood test
- people who are participating, or have previously participated, in a clinical trial involving an HIV vaccine, since the test could produce a false positive result.
When should you take the test?You need to wait 12 weeks after a possible exposure to HIV before using the oral self-test if you want a reliable result.
The test detects the antibodies your immune system produces to fight the virus. However, it can take up to 12 weeks for those antibodies to build up to a level that can be detected by the self-test.
If you take the OraQuick self-test before the recommended 12 weeks and the result is negative, you should not consider that result final. You will need to repeat the test once the 12 weeks have passed for the result to be reliable.
If the result is positive, no matter when you took the test, you do not need to repeat the self-test. Instead, make an appointment with a healthcare professional for a confirmatory blood test.Possible HIV exposures include:
- anal, frontal, or vaginal sex without a condom with a partner living with HIV whose viral load is detectable, or with a partner whose HIV status is unknown;
- sharing equipment used for drug injection.
Should you do it alone or with support?One of the benefits of the HIV self-test is that you can choose how you want to do it: on your own, at home, with someone you trust, or with the support of a community worker.
A community worker can guide you through the process, help you interpret the result, and support you afterwards if needed.
Support options vary from one organization to another and may be available online, by text, by phone, or in person.
To find support near you, use the postal code search tool to locate the nearest community HIV resource.
How can you get the oral HIV self-test?
The OraQuick oral HIV self-test was approved for use in Canada on February 10, 2026. At the moment, it can only be ordered in bulk, with a minimum order of 25 tests at a time. It may eventually become available for individual purchase or through certain community organizations.
The cost is 20 Canadian dollars (CAD) per test, plus taxes and shipping.
To order it, you need to complete an online form at reach4testing.com.Oral self-test or blood self-test?
There is another type of HIV self-test: the INSTI blood self-test. It involves analyzing a drop of blood and gives a result within one minute.
Learn more about the blood self-test in the above section.
- Informing your partners
One day you may be faced with having a conversation about the fact that you’ve contracted an STBBI. It can be a difficult topic to bring up. Often our partners react by accusing us of being the source of the infection. As much for HIV as for other STBBIs, there are different ways to inform your current and previous partners, and deal with negative reactions:
Here are a few suggestions that might help:
- Prepare for your meeting or call by thinking ahead about what you plan to say
- Choose a time when your partner will be able to give you their undivided attention
- If you break the news by phone, make sure it is a good time to talk before you broach the topic
- If you break the news in person, choose a neutral, quiet and safe location where you can speak without being disturbed
- Keep it simple:
- The name of the infection you have
- That a person can be infected even if they don’t have symptoms
- That it is essential that they see a doctor (or nurse) quickly to get tested, be evaluated, and get treated, as the case may be
- Invite your partner to learn more about chlamydia, gonorrhea, syphilis or HIV by giving them fliers, or suggesting that they visit sante.gouv.qc.ca (website for the general public) or itss.gouv.qc.ca (website for youth)
- Give them the notification card that your doctor or nurse provided you. This card contains information on the infection you have contracted, and provides useful references
- Encourage your partner to see a doctor
- If your partner accuses you of being the source of the infection, remind them that looking for someone to blame solves nothing. The important thing is that they get tested, and stay healthy
Getting help from a doctor or nurse
Some people do not feel comfortable, for a number of reasons, telling their current and previous partners themselves. If this is the case for you, a healthcare professional can notify your partners for you. They will ask you for information (your partner’s phone number, for example) then will attempt to anonymously make contact and suggest that they see a doctor.
You can also visit the website of the Portail VIH/sida du Québec (in French only), which offers the option of anonymous, confidential and free notification of your partners.
Receiving a disclosure
You might also find yourself in the reverse situation: your partner reveals that he or she has an STBBI. It is normal to feel worried and upset by what the person has told you. However, remind yourself that this information was shared with you because that person was worried about your health and wanted you to be able to be treated quickly if necessary.
- Negotiating and using condoms / dental dams
Condoms are not the only way to avoid getting HIV and other STBBIs, but they are certainly the best known and most accessible. They are also highly effective against HIV and hepatitis. However, the desire to use them could lead to delicate situations where you want to use one, but your sexual partner does not. Here are a few suggestions to help make that discussion easier:
Fear is one factor that sometimes prevents us from talking about condoms:
- Fear of what the other person will think
- Fear that the other person thinks differently about using them?
- Fear that the other person will think that you are sleeping around, or are being unfaithful
- Fear that the other person will refuse, or argue with you
- Fear that the other person will think that you have an STBBI
If using a condom is important for you, here are a few strategies to help you broach the subject. Who knows? Maybe your partner wanted to talk about it too… but was too shy to bring it up.
You can help your partner understand that using a condom is non-negotiable by:
- Always having condoms on you (in your purse), and in every room of your home
- Leaving condoms and lubricant in sight, on the night table, for example
- Giving your partner a condom before any form of penetration
If you choose to talk about it before hand, here are a few tricks to facilitate the conversation:
- Bring it up before sex is initiated, in a calm environment that lends itself to talking about it, during dinner, for example
- Be aware of the reasons you want to use a condom. Write them down. It is easier to negotiate when you know what you want
- Talk about it with your friends. They might have some ideas that could help you talk about it
- Think of a situation when you had to negotiate using a condom. What challenges did you come up against? How did you overcome them?
Emergency contraceptive pill
In situations where a condom was either not used or broke during sex, emergency contraception (the morning after pill) can prevent unplanned pregnancy if taken right away. Although it is possible to take it up to five days (120 hours) after unprotected sex, it is recommended to take it as soon as possible to maximise effectiveness. for maximum effectiveness it is better not to wait. This is available without a prescription in pharmacies.
Post-exposure prophylaxis (PEP)
In situations where a condom was either not used or broke during sex, and you believe there is a risk of HIV infection, you should be aware that there is a treatment that can minimise the risk of HIV infection. See a doctor immediately or visit the ER.
- Reducing risk in your sexual practices
Sexuality can be expressed in many ways. Sexual practices are just as numerous. From kissing to kink, there are ways to reduce the risk of contracting STBBIs, including HIV.
Touching, kissing, massaging
Stimulating the erogenous zones by touching, kissing, massaging, enjoying a bath together, etc. are all activities you can practice with no reservations. They involve no risk of HIV transmission.
If you insert your fingers in your partner’s anus or vagina, keep your nails short and filed to avoid cuts. You could also use latex or vinyl gloves and lots of lubricant for this type of activity.
Genital to genital contact presents a negligible, even non-existent risk of HIV infection. In fact, there is very little risk of HIV transmission during sex between women, except during your period or if you engage in activities involving blood. There is, however, the risk of transmitting other STBBIs. If this is a practice you enjoy and do often, make sure you get tested regularly.
Oral sex
To protect yourself and reduce risk:
- Keep your mouth clean and avoid oral sex if you have cuts, lesions, ulcers, gingivitis (inflammation of the gums), or other infections in your mouth.
- Avoid oral sex on a day when you have been to the dentist.
- Avoid brushing your teeth, using dental floss, or using mouthwash for an hour before and an hour after oral sex. This will minimize the possibility of lesions, irritations, or blood in your mouth.
- Avoid getting semen or vaginal secretions in your mouth.
- When you are being tested for sexually transmitted and blood-borne infections (STBBIs), ask the doctor to take a sample from your throat.
- sing a condom or latex square (dental dam) for oral sex is another way to minimize risk. Flavoured ones exist, as well as those without lubricant.
Vaginal and anal sex
To reduce risk:
- Correctly use a latex, polyurethane, or polyisoprene condom for vaginal and anal penetration.
- Use water- or silicone-based lubricant. Do not hesitate to reapply, as this reduces your risk of lesions. Be careful! Oil-based lubricants are not compatible with latex condoms. This information will be indicated on the package.
- If you are practicing vaginal and anal sex, remember to change condoms when you change orifices to avoid transmitting bacteria from the anus to the vagina.
- Flavoured condoms can be used for penetration. However, some women may be prone to infections as a result. Flavoured condoms are best kept for oral sex.
- Remember that condoms also protect you from unplanned pregnancies.
- When you are being tested for STBBIs, ask your doctor to take a sample from the anus if you practice anal sex.
- For cultural reasons or personal hygiene, some women use vaginal douches or other substances to clean their vaginas before or after sex. These substances can irritate the mucus membrane of the vagina and potentially increase your risk of STBBIs. It is recommended that you wash your vagina daily with water, nothing else.
There are other prevention strategies, including PrEP and PEP (see the Treatment as Prevention section).
Kink
Role-playing games and sadomasochism are not high-risk practices for transmitting HIV and other STBBIs. You can play out your favourite scenarios safely, as long as you stick to the precautions mentioned on this site, depending on which sexual activities are involved.
Hardcore practices that can cause bleeding or lesions on the surface of the skin, as well as practices involving surgical tools, can involve the risk of bacterial infection and, in some circumstances, the risk of transmitting of hepatitis C and HIV. Make sure you are familiar with basic precautions you should be taking, and play out your scenarios with an experienced partner.
Sex toys (Dildo, butt plug, vibrator)
A sex toy has the same potential for transmitting an infection as a penis. If you plan on sharing toys, it is important to put a condom on them. In addition, if you and your partner decide to go from vaginal penetration to anal penetration, you should change condoms.
Toys are often porous, which means that viruses and bacteria can get trapped. After each use, make sure to clean your toys thoroughly. You can use dish soap and hot water, making sure to rinse well. Specialized stores also sell cleaning products specifically designed for different types of toys. Depending on what they’re made of, you can boil them to sterilize them.
- Treatment as prevention
In addition to vaccines for certain sexually transmitted and blood-borne infections (STBBIs), there are a few HIV prevention methods based on pharmaceutical treatment. Depending on the type of sexual behavior you engage in, they could be used before or after high-risk sexual activity.
Vaccines
There are currently vaccines for hepatitis B and the human papilloma virus (HPV).
The hepatitis B vaccination program in schools means that many people have now received this vaccine, which is known to be effective for life. If you have not been vaccinated or are not sure if you have been, speak to your doctor.
The HPV vaccine has been offered to young girls and boys in schools for a number of years now, and to women with weakened immune systems or who are living with HIV. Its effectiveness is highest if it’s given before a person’s first sexual relations or before age 26. Speak about it with your doctor.
Post-exposure prophylaxis (PEP)
PEP, for post-exposure prophylaxis, is a treatment available if you have had unprotected vaginal or anal sex with a partner whose HIV status is positive or unknown. Your doctor will evaluate your risk level before prescribing this treatment.
In order for this treatment to work, it needs to be initiated as quickly as possible and no more than 72 hours after the risk occurs. Not all healthcare professionals are familiar with this treatment, particularly those who are not specialized in HIV. In view of this, it is strongly recommended that you visit a clinic specialized in HIV and sexually transmitted and blood-borne infections (STBBIs).
You can make an appointment in a specialized clinic or go to the ER of your nearest hospital. Remember that it is important to be seen as quickly as possible within the first 72 hours after the high risk sexual activity takes place. Do not hesitate to call your local community HIV organization for guidance.
Pre-exposure prophylaxis
You may also have heard of PrEP, or pre-exposure prophylaxis, an HIV treatment used to prevent infection before it happens.
In Québec, PrEP is provided to people who are at high risk of being infected with HIV. For instance, it’s offered to couples in which one person is living with HIV and the other is not. In this context, PrEP can be a way to prevent infection.
To have access to PrEP, you need a prescription from your doctor.
Viral load and non-transmission of HIV
In the last few years, many scientific studies have shown that effective treatment, taken as prescribed for at least six months, prevents the sexual transmission of HIV.
Several measures serve to monitor the development of the HIV infection. One of these measures is viral load, meaning the quantity of HIV in the blood. It’s measured in number of virus copies per millilitre of blood. The risk of transmitting HIV fluctuates with the viral load: the lower the viral load, the lower the risk of transmission.
As soon as a person living with HIV begins to take effective treatment against the virus, the viral load drops considerably. When you take treatment without missing any doses, go for regular medical follow-up, and maintain your viral load at a very low level, HIV will not be transmitted.
HIV non-transmission is a recent development which comes from advances in treatment as well as the conclusions of major international studies. The scientific community has come to a consensus on this along with the HIV prevention field as a whole and public health agencies the world over.
In Québec, the Ministère de la Santé et des Services sociaux affirms that there is no proof of HIV transmission from oral, anal or vaginal sexual relations without a condom when:
- The person living with HIV takes their treatment as prescribed
- The quantity of virus in the blood is measured (viral load measurement) every four to six months
- The quantity of virus is maintained at a very low level, meaning below 200 copies per millilitre of blood.
For more information on this subject, speak with your doctor.
It is important to remember that, though this is the position of Quebec public health, it does not protect you from the risk of criminal prosecution if you have not told your partner(s) that you are HIV-positive. For more information, see the section of the COCQ-SIDA website (in French only) on criminalization of HIV exposure or the website Pouvoir partager / pouvoirs partagés (French).
Do I still need to use a condom?If you are in a relationship and meet the above-listed conditions, the choice is yours. However, we suggest that you and your partner meet with a doctor beforehand to discuss your options before making a decision.
Antiretroviral therapy and condom use are both recognized as effective strategies for reducing the transmission of HIV. Condoms also protect you against other STBBIs and unplanned pregnancies.
- Drug use and sex
Mixing drug use and sexuality can make you feel good. However, be conscious of the fact that drugs can affect the way you perceive risk. Be aware of the risks, find ways to reduce or avoid them, establish your limits, and prepare yourself accordingly. When your judgment is impaired, you will be glad you did.
Some advice:
Make sure you have plenty of condoms and lubricant (have a few different kinds in your purse, for example). If the condom breaks or does not get used, plan to take emergency oral contraception and, if needed, post-exposure prophylaxis.
Plan to bring enough materials to inject or inhale drugs. Better to have too much on you than to run out in the middle of the party. You can get injection kits in select pharmacies and community organizations.
Sharing works such as straws, syringes and stericups presents a risk of transmitting HIV and hepatitis C. We recommend not sharing them.
If you like to mix drugs, read Le Blender (French) a guide created by the AQPSUD (French) on mixing drugs and the associated risks.
If you are living with HIV, prepare your treatment doses before taking any drugs, and find a way to remember to take them, maybe by setting an alarm on your phone. Remember that certain anti-HIV medications, like Ritonavir, enhance the effects of drugs. Wait at least 30 minutes after taking Ritonavir before taking any drugs, and start with a half dose.